
Innovative immersion program focuses on healthcare workforce gaps today, student career options tomorrow
Immersion innovation is ‘triple winner’ for patient care; student experience; today's workforce gaps
It's a triple winner to tackle a triple threat.
In this case, the ‘trifecta’ program launching this summer is the “Healthcare Exploration in Patient Care” program, an undergraduate immersion opportunity for University of Cincinnati students in partnership with the affiliated health system, UC Health.
The program has promise to become a national model due to widespread challenges in
- Recruiting entry-level healthcare workers;
- Tightening admissions standards to medical schools and other advanced study programs related to healthcare;
- Need to retain healthcare professionals for the long term (so that their experience continues to serve patients).

Arthur M. Pancioli, M.D.
According to Arthur M. Pancioli, MD, UC Health physician and the Richard C. Levy Chair of the Department of Emergency Medicine at the UC College of Medicine. “In a nutshell, these simultaneous challenges are actually one another’s solution and why we crafted this healthcare exploration pipeline to launch quickly, in fact, as a pilot this summer.”
Pancioli is the originator of the program’s concept, working in tandem with other administrators, faculty, healthcare providers and students to bring the program to the starting gate.

UC College of Arts and Sciences student Chelbi Hill, 20, of Indianapolis, is majoring in pre-medicine and psychology. Here she stands next to a computer monitor where she charts patient data. Says Hill: "This program has given me so much insight into the realities of the hospital and healthcare setting. It allows me to get a feel for taking care of patients, working with other healthcare workers, and properly functioning in a hospital setting. This experience has confirmed my love for healthcare, and I have become more comfortable with the idea of me being in this setting as a profession." Photo by Colleen Kelley.
UC/UC Health: integration of resources and opportunities
“I’m a huge believer in the combined UC/UCH missions. Every time we can increase the integration of our missions, we will find big wins,” affirms Pancioli, adding. “To be the very best as an Academic Health Center on behalf of Cincinnati, we need to amplify resources and opportunities that will strengthen both institutions and our region overall. This checks all the boxes on our mutual and wider education, training and workforce needs, and it will help patients. In every respect, this kind of model is our future.”

UC medical sciences undergraduate Kayla Lux folds laundry in the neonatal intensive care unit. Specifically designed for undergraduates at UC, the 'Healthcare Exploration in Patient Care' program provides students with paid patient care experience, while the health system fills positions and recruits entry-level workers. According to program originator Art Pancioli, M.D., the effort is "transformational for the students and for the patient care setting too. The energy and motivation of the UC students is high octane and exuberant." Photo by Colleen Kelley.
Original impetus: "We don't have enough nurses"
The “Healthcare Exploration in Patient Care” program was first fast tracked by Pancioli; Valerie Hoagland-Scarfpin, UC Health assistant vice president, talent acquisition; Alex Maus, UC Health director of educational placements; and Anil Menon, UC College of Medicine associate dean and director of the undergraduate medical sciences program, in the closing days of 2021. They also engaged with others at UC Health like Teri Grau, chief nursing officer and vice president of nursing.
Pancioli recalls, “I began ruminating that we all know we don’t have enough nurses in this country. Overall, the workforce issues in healthcare are severe, and this isn’t going to change anytime soon. So, our old models really don’t apply anymore. We need to restructure our healthcare workforce. For instance, specialization in nursing roles, whether an operating room nurse or an ICU nurse or psychiatry nurse or in another role or unit, is now a required norm to best serve our patients. These are distinct, complex roles where highly trained and skilled nurses need to focus on care needs at or above the threshold of their full capabilities. Given that, I began mentally recalculating the care model entirely, and when you’re trying to redesign a model, you ask yourself what and how can you redeploy assets. How could we provide those nurses more support staff?”
I'm a huge believer in the combined UC/UCH missions.
Art Pancioli, M.D., UC professor of emergency medicine, and chair, UC Health Department of Emergency Medicine

UC Health registered nurse Felicia Kramer, left, walks in the neonatal intensive care unit with UC College of Medicine's Kayla Lux, who is an undergraduate student in the medical sciences program and a participant in the new healthcare exploration program. Photo by Colleen Kelley.
Grau quickly agreed to help launch the new program, stating, “I think it’s a great opportunity for students, great for nurses and great for patient care.
“This will be a benefit to nursing staff and our patient care specifically, as we follow an approach we call team nursing. We work as a team. It’s a means for allowing nurses to work at the top of their license (meaning to the full level and extent of their education, training and experience versus more routine tasks well below skill level). The team approach allows others on the care team, like patient care assistants, therapists and others, to conduct the important care practices most appropriate for their skill sets,” she states, adding, “It’s a win-win-win. And we’ll get a lot of feedback from our nurses, so it’s successful for everyone, and most of all, for the patients.”
Participating student Robert Heins, 21, a health sciences major in UC’s College of Allied Health Sciences, who is from Mansfield, Ohio, states, “I do believe that I have been making a difference in both helping patients and the healthcare team. Last week, I was thanked by a family for being attentive…just treating the patient how I would want my own family to be treated. I’m with patients in the cardiac division, so they require an immense amount of recovery and rehab. I have found myself simply talking with these patients and giving them much-needed company. I truly enjoy helping these patients progress along the road of recovery. Additionally, the staff on my floor has thanked me multiple times for the help I have provided.”
Student Chelbi Hill, 20, a pre-medicine and psychology major from Indianapolis, says much the same: "I believe I am making a difference because there are patients and families that remember me by name, and they light up when I enter the room. I think that is really important in this field because the hospital can be uncomfortable for most people. I make a difference with the healthcare team by assisting them with their tasks... ."
...it's a great opportunity for students, great for nurses and great for patient care.
Teri Grau, chief nursing officer and VP of nursing, UC Health

UC College of Arts and Sciences student Martin Ogbebor, left, is a participant in the new 'Healthcare Exploration in Patient Care' pilot program. Here, he works with registered nurse Will McDaniel. Photo by Colleen Kelley.
Changing landscape for medical school admissions
Menon, who heads one of the nation’s first undergraduate medical sciences programs (founded at UC to provide a diverse gateway major into medical, dental, pharmacy, optometry, public health, or business administration, research or other related fields), explains, “In applying to medical school, pharmacy school, dental school or an array of allied health programs like a physician assistant master’s program, there is – increasingly – some expectations for applicants to demonstrate a substantial immersive medical experience. Medical schools and other specialty preparatory programs are becoming very savvy in this regard. They’ve come to realize that, too often, applying students had never really worked in a hospital or clinical care setting. They only really knew what they’d seen on TV.”
They (students) only really knew what they'd seen on TV.
Anil Menon, UC College of Medicine associate dean; director, undergraduate medical sciences program
Currently, the American Association of Medical Colleges (AAMC) strongly recommends that applicants gain exposure or experience via clinical shadowing or a hands-on health exploration. (And many programs to train physician assistants (PA) require applicants to demonstrate a high number of hours – 1,000 or more – of healthcare experience.)
It turns out that when undergraduate students have four straight years of academic training at the baccalaureate college level and then go into a medical school or related program, there are those who realize late into their advanced studies or perhaps in residency or even in medical practice that the realities of the field are not a good fit for them. Explains Menon, “Based on AAMC data, we know that these folks, often, due to issues of sunk costs and family or other expectations, may know they are not as fulfilled as they might be but then still work a decade or so and only then step out – carrying valuable experience out of the profession.”
Because of the personal and professional time and energy as well as financial resources ultimately required to complete health training and launch and carry forward service careers, medical schools and other allied health programs are expressing increasing interest in applicants’ authentic, hands-on experience as part of the application and admission process. In other words, it’s no longer always enough to have shadowed a physician. The requirement for a substantial immersive experience has been rather loose until now, but it’s increasingly becoming a codified requirement in more and more programs.
UC College of Allied Health Sciences student Grace Dinkelaker takes a blood pressure reading. Photo by Colleen Kelley.
UC's medical sciences undergraduate program
This very reality was behind the founding of UC’s medical sciences undergraduate program in 2012 and the “Healthcare Exploration in Patient Care” program this summer. (UC’s medical sciences undergraduate attracts up to 1,000 applicants from 26 states, accepting only 100 each year.)
Says Menon, “Most academic programs preparing students for medical, dental, or pharmacy school are what I call ‘opt-in.’ In other words, without a whole lot of authentic background regarding the realities of healthcare, you opt in. Our medical sciences program is more of an opt out. Combined with your initial interest in medicine as a career field, we try to give you lots of exposure so that at the time of your undergraduate graduation, you have the chance to opt out of any particular part of the medical field that’s not right for you before you spend years on a medical school education.”
And the new “Healthcare Exploration in Patient Care” opportunity is a next step toward formalizing the learning and hands-on opportunities for undergraduates (though the new “Healthcare Exploration in Patient Care” is open to UC undergrads beyond the medical science undergraduate program.)
We need earlier pathways for undergrads to enter the health care arena.
Anil Menon, associate dean and director, undergraduate medical sciences program
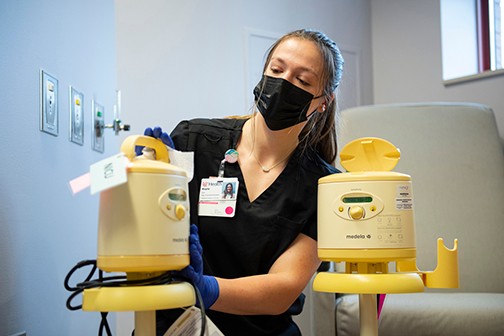
UC's Kayla Lux. an undergraduate student in the medical sciences program and participant in the healthcare exploration program, cleans breast pumps in the neonatal intensive care unit. Photo by Colleen Kelley.
The overall goal is that undergraduate students interested in healthcare benefit from an immersive medical experience to round out their decision making process about what they might want to do as they advance. States Pancioli, “We need earlier pathways for undergrads to enter the health care arena in a way that will be meaningful and real for them, with legitimate work that shapes their thought process for decision making and provides the health system with the best and brightest of team mates to buoy up the basic care giving model.”
Grau echoes him, “Working with patients is a blessing. It’s people at their most vulnerable moments, and some students may not have as much experience at that level. It’s very important to see that and to see what that’s like.”

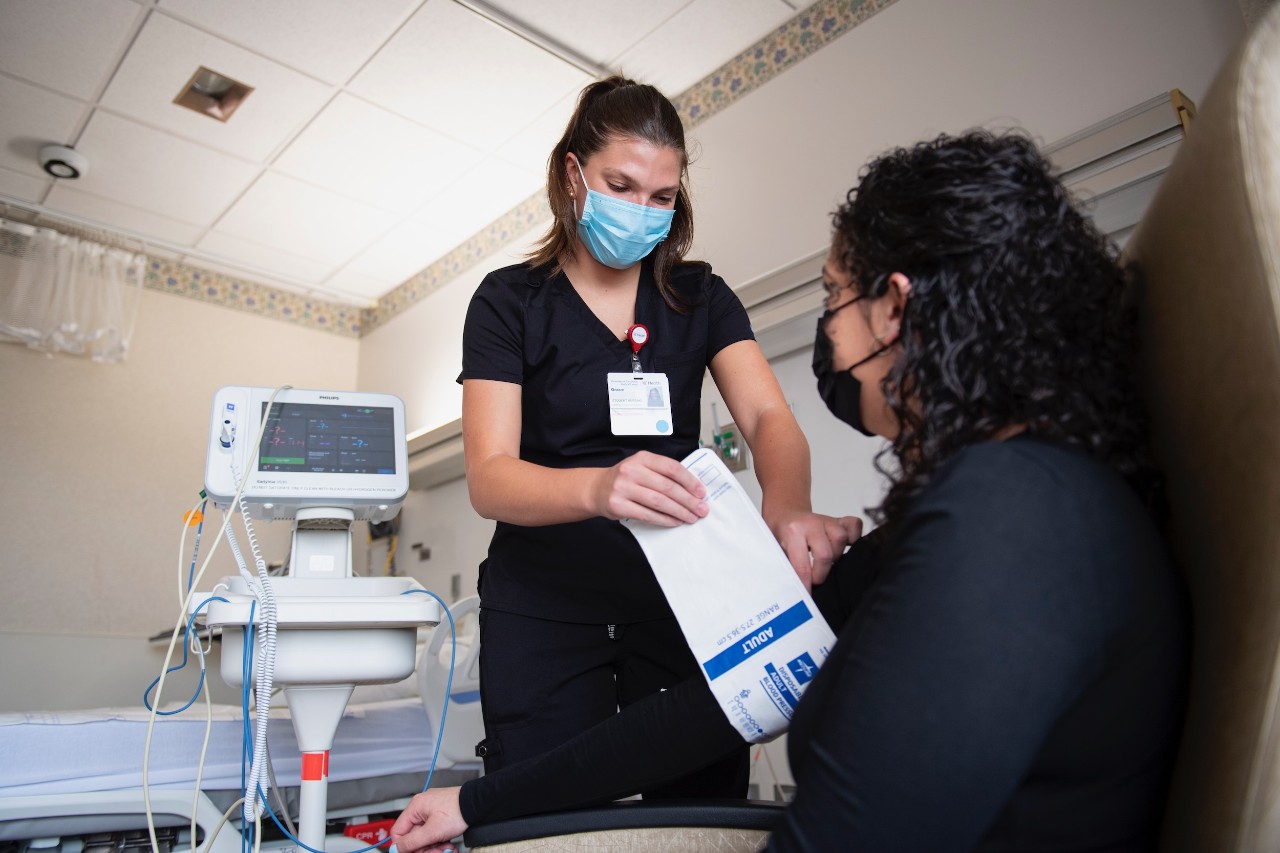
UC student Chelbi Hill, at left, confers with UC Health staff Britny Wilford, center, and registered nurse Meghan Carter. Carter is supervising Hill as part of the 'Healthcare Exploration in Patient Care' program. Hill says she was initially interested in the program because of the range and scope of experiences it offered: "This sounded like a great opportunity because not very many programs allow students to care for the patients in a hands-on approach." Photo by Colleen Kelley.
Healthcare exploration pipeline: academics + real world experience
For the summer 2022 pilot, 59 students were accepted to work full time at $17 an hour. Then, in the coming fall and spring terms, 150 students will work 18 hours a week and participate in a seminar class with guest speakers, required readings and reflection papers. Participating students who successfully compete both the hands-on work and academic requirements will not only receive pay but 3 credit hours, a confirmatory note on their academic transcripts as well as a letter of recommendation from their college leadership.

UC student Grace Dinkelaker of Hamilton, Ohio, is participating in the 'Healthcare Exploration in Patient Care' program, which provides students with paid patient care experience, while the health system fills positions and recruits entry-level workers. Photo by Colleen Kelley.
Says Grau, “This pilot and program are really aligned with our mission as an academic teaching facility too. It’s another avenue by which our future health care professionals can come into the industry and to UCMC. For me, long-term success would be like our ‘Match Day’ that we already have for residents, but we have a ‘Match Day’ for students in this Health Exploration program. They get a lot of different exposure to the roles and the disciplines, and ultimately, they graduate, and we’re able to offer them a next step or a future with UCMC that’s a match for them personally and professionally.”
Initial applicants to the “Healthcare Exploration in Patient Care” opportunity represented allied health, arts and sciences, medical sciences, nursing and pre-pharmacy majors at UC. The students were able to rank their first-choice work areas, including general medicine, surgery, psychiatry, women’s health, cardiology and neurology.
The UC students are working as patient care associates (PCAs), providing both comfort and some very basic clinical care. Again, these PCA positions help enable nurses to work at the top of their licensure. PCAs deliver food and help patients eat and drink, help with bathing and bathroom visits, conduct catheter care, take vital signs, test range of motion, remove and reapply splints and braces, change dressings or compresses, help position oxygen masks, empty drainage bags, conduct specimen collection and more.
I wish I would have had this opportunity as an undergrad to do something like this.
Alex Maus, UC Health director of educational placements
UC Health’s Hoagland-Scarfpin emphasizes, “For the students, it’s their triple win too. You’re going to get paid. You’re going to get credit hours. You’re going to get this exposure backed up by a recommendation letter to help you to the next level if that’s where you want to go.”
“I wish I would have had this opportunity as an undergrad to do something like this,” adds Maus, who worked as a physician’s assistant (PA) before entering the education side of health (and as a PA applicant, was required to show significant hands-on experience in order to apply and enter the PA master’s program).
Student Heins, who plans to continue in the program for the next year with the goal of attending medical school by Fall 2023, agrees, “When it was announced, this program stuck out to me as it was more than just the typical job that someone our age can obtain. We are able to work in multiple specialties as we progress though the semesters and can progress to the emergency department or to once of the ICUs. This mobility and never-ending possibilities to learn is what really attracted me.”
The business bottom line

UC College of Arts and Sciences student Martin Ogbebor of Miamisburg, Ohio. Photo by Colleen Kelley.
The business model to support the new program is seamless, as it’s already in place, according to Hoagland-Scarfpin. There is no impact to the fiscal bottom line because the students are actually filling open (already funded) positions that are very much ready to hire among the public. (In fact, the students could conceivably have entered these jobs simply by filling out the public-facing application.)
There are currently about 1,300 entry level UC Health job openings at three locations in Cincinnati, including entry level patient care associates, which is the job and role the UC students are filling. Thanks to the “Healthcare Exploration in Patient Care” program, it’s estimated that in the next year, the program will supply approximately 100,000 work hours to the healthcare system.
Featured image at top includes leadership members of the 'Healthcare Exploration in Patient Care' program as well as participating students in this inaugural summer pilot. From left are: College of Allied Health Sciences student Robert Heins; College of Medicine undergraduate Tripura Vithala; UC Health director of educational placement Alex Maus; program originator Art Pancioli, M.D.; associate dean Anil Menon, director of the undergraduate medical sciences program; vice president of nursing and chief nursing officer Teri Grau; and College of Arts and Sciences student Dwijen Shah. Photo by Colleen Kelley.
Beyond the classroom
UC invented cooperative education more than 100 years ago, and we continue to innovate all aspects of experience-based learning, including internships, service learning, virtual co-ops, community projects and industry partnerships. UC co-op students earn (a collective $58 million annually) while they learn - one reason UC co-op is top-ranked in the nation.
UC students: The current summer and the upcoming Fall 2022 'Healthcare Exploration in Patient Care' programs are full. Applications will be accepted after Labor Day (Sept. 5, 2022) for the Spring Term program beginning in January 2023. The application link will be placed here when it is available, so please revisit this story after Sept. 5, 2022.
Related Stories
UC celebrates record graduating class at commencement
April 25, 2024
UC celebrated its doctoral hooding and master's recognition ceremony at Fifth Third Arena as part of its three-day commencement for the largest graduating class in university history.
2024 Daniel Drake Medals to be awarded April 27
April 24, 2024
The UC College of Medicine will award three people with 2024 Daniel Drake Medals April 27.
From literature to AI: UC grad shares career path to success
April 23, 2024
Before Katie Trauth Taylor worked with international organizations like NASA, Boeing and Hershey, and before receiving accolades for her work in the generative AI space, she was in a much different industry: English and literature.
