
COVID vaccinations lag in rural, underserved communities
UC study points to severe health care disparities in United States
Vaccine hesitancy is just one reason fewer people in some parts of the United States have been inoculated against coronavirus.
A study in the journal Lancet Regional Health found that wide disparities in health care coverage, particularly in rural areas, hampered vaccination efforts during the COVID-19 pandemic. The findings point to a hidden divide in America between those with geographic and financial access to doctors, hospitals and clinics and those without.

Diego Cuadros. Photo/Provided
University of Cincinnati epidemiologist Diego Cuadros led an international team of researchers investigating disparities in vaccination rates across 2,417 U.S. counties. They found that the availability of health care resources influences vaccine coverage.
The pandemic has killed more than 6.3 million people worldwide, including more than 1 million people in the United States alone. When it comes to the country’s comparatively high rate of mortality, researchers point to failures of vaccination compared to other countries.
Cuadros, an associate professor of geography in UC’s College of Arts and Sciences, said the rate of vaccination varies widely across the United States. While some people may be reluctant to get vaccinated because of unfounded fears or misinformation, that tells only part of the story, he said.
“Areas with low vaccination uptake had low health care infrastructure and barriers to access to health care,” Cuadros said. “During the pandemic we realized the huge health care disparity we have in this country.”
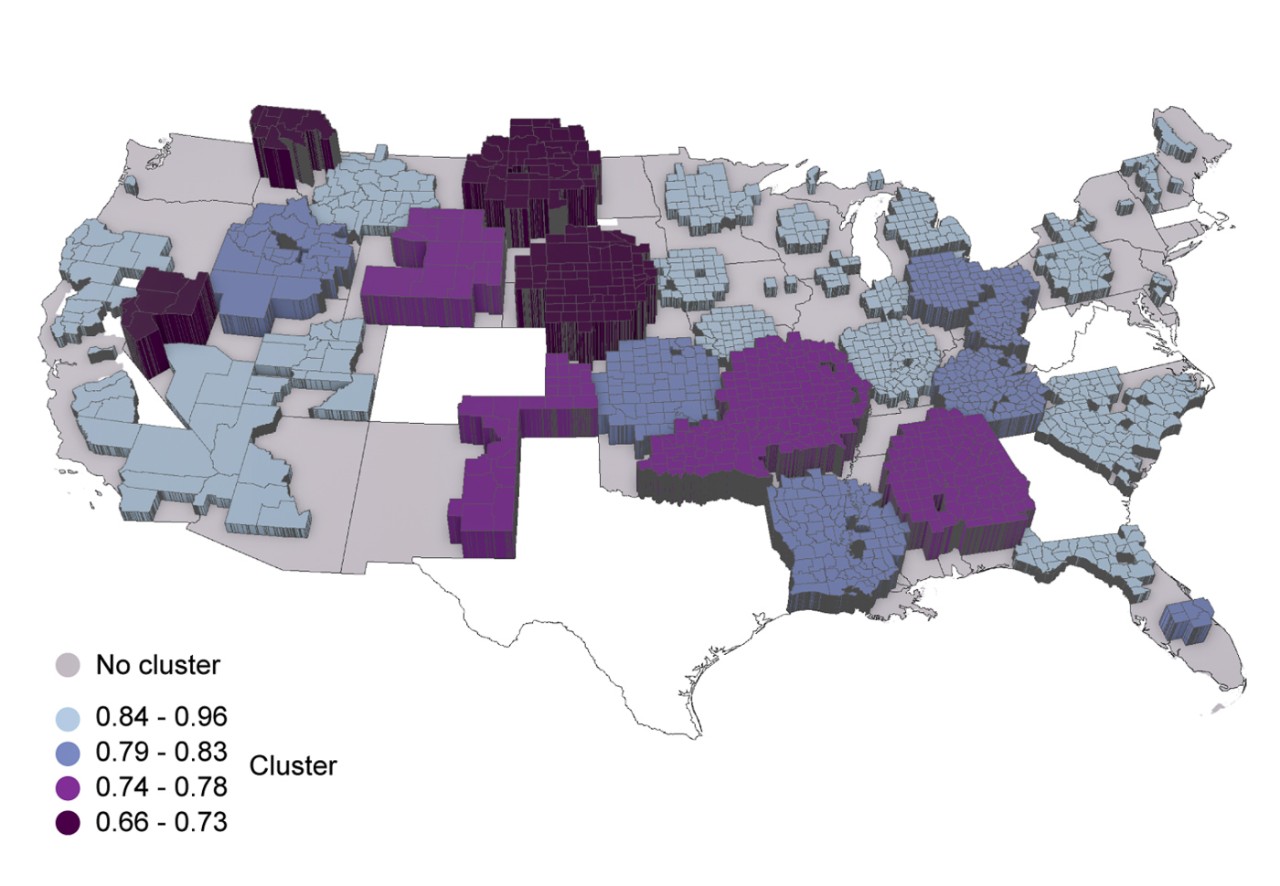
A map of vaccine coverage in the United States shows rates of vaccination. The darkest colors of purple reflect the lowest rates of vaccination. Graphic/UC Digital Epidemiology Lab
Barriers to health care access include cost, insurance coverage and transportation.
In national surveys, about 20% of the U.S. population has reported an unwillingness to be vaccinated. This does not account for the larger unvaccinated population. While more than half of the population in every U.S. state is now fully vaccinated, some states are much further ahead than others.
Cuadros said areas with low vaccination saw the highest rates of mortality from the virus during the delta and omicron waves, demonstrating the terrible impact that health disparities can have on underserved communities.
Our study suggests clear disparities that need to be addressed.
Santiago Escobar, UC geography student
Ironically, the United States is considered the most capable country in the world to prevent a pandemic based on the Global Health Security Index. It also ranks high in detection, response and public health. But the United States has wide county-by-county disparities in public access to hospitals and doctors, health insurance coverage and healthcare funding.
UC’s analysis found that people in underserved communities were as much as 34% less likely to be vaccinated against COVID-19. These included counties in Nevada, Montana, North Dakota, South Dakota and Nebraska where vaccination rates were lowest.
“America’s healthcare system has improvements to be made to address historical disparities that, as shown in our study, can influence individual-level decision-making,” study co-author and UC geography student Santiago Escobar said. “Our study suggests clear disparities that need to be addressed.”

UC College of Pharmacy student Kyle Schuchter draws a COVID-19 vaccine during a drive-through clinic at UC Health in this 2021 file photo. Photo/Colleen Kelley/UC Marketing
Co-author Phillip Coule, M.D., chief medical officer for Augusta University Health in Georgia, said the study underscores the impact of vaccination in fighting diseases like COVID-19.
“Those responsible for guiding health policy need to consider issues such as vaccination rates, access to care and health disparities when evaluating outcomes from COVID-19 and other conditions,” he said.
Co-author Neil MacKinnon, provost for Augusta University, said the pandemic caused enormous disruptions to health care services even in places with ready access. People saw their doctors much less frequently, leading to more undiagnosed cases of cancer and other diseases.
“Our study demonstrates that these disruptions were not uniform across the United States,” said MacKinnon, former dean of UC's College of Pharmacy. “Many counties, especially those in rural areas, experienced significant disruptions in health care, including the distribution of the COVID-19 vaccine itself.”
Rural communities face challenges that exacerbate the lower rates of COVID-19 vaccination such as restricted access to testing, vaccine supplies and fewer health care workers, researchers said.
The study was supported by UC’s new Digital Futures initiative in a collaboration with researchers from the University of Santander, Colombia; the University of Washington School of Medicine; the University of Hawaii; the International Initiative for Impact Evaluation, Zimbabwe; Hokkaido University in Japan and Augusta University.
Featured image at top: UC College of Pharmacy student Kaitlin Kuznacic administers a COVID-19 vaccine during a drive-through clinic at UC Health in this 2021 file photo. Photo/Colleen Kelley/UC Marketing
Related Stories
A jolly good trip: Bearcats take on London for fragrance company
May 15, 2026
Six NEXT Innovation Scholars at the University of Cincinnati traveled to London to transform field research into actionable recommendations for British luxury bath, body and fragrance brand Molton Brown.
Driven by curiosity, guided by care
May 14, 2026
Max Wilson, a University of Cincinnati College of Allied Health Sciences health sciences major on the pre-physician assistant track, found his path expanding beyond the classroom and into hands-on research focused on human performance and patient care.
UC Blue Ash celebrates top students and recognizes Honor Student of the Year
May 14, 2026
The University of Cincinnati Blue Ash College recently hosted a special event that celebrated students for exceptional achievements during the 2025-26 academic year. The honorees included academic award winners, student engagement award winners, Latin Honors graduates, and the 2026 UC Blue Ash College Honor Student of the Year.
