UC engineering students help Venti-Now develop low-cost ventilators
Students gain experience with Cincinnati nonprofit launched in response to pandemic
Two biomedical engineering students are making a tangible impact working with Venti-Now, a nonprofit start-up company launched in Cincinnati in response to the COVID-19 pandemic to develop a new low-cost ventilator.
UC students Jacquelyn Chapman and Johnathan Wisecarver have been working with Venti-Now for the last few months developing a reasonably priced ventilator for low-resource areas. Under the direction of their biomedical engineering professor, Peter Campbell, who lends his expertise as medical team leader for Venti-Now, the students have worked alongside experienced professionals to make a difference during the pandemic. UC Health and UC's College of Engineering and Applied Science helped provide Venti-Now with medical testing and consultation.
Both Wisecarver and Chapman viewed their work with Venti-Now as a once-in-a-lifetime experience. Chapman, who will graduate from UC in 2021, joined the company as part of the College of Engineering and Applied Science (CEAS) cooperative education (co-op) program.
“Dr. Campbell described the opportunity and I thought it was perfect for acquiring knowledge and experience that often takes a few years at an entry-level position to be given the same caliber of work,” Chapman said.
Chapman had the opportunity to help prepare documents for submission to the U.S. Food and Drug Administration, analyze test data and assist with clinical reviews, among other responsibilities.
“I appreciate the connections that UC has facilitated to grow as I have in this role with Venti-Now,” Chapman said. “I truly believe that experience is the best way to solidify the material you have learned in your coursework. While acquiring your degree, co-op allows you to figure out exactly what you like best and how you fit best in the industry, which often takes people years to figure out postgrad.”

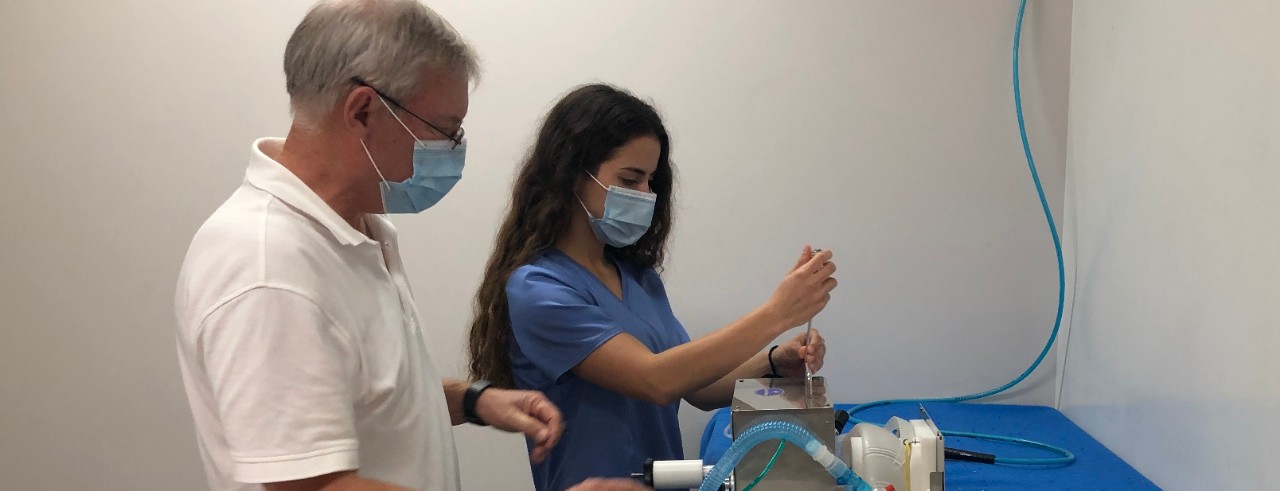
Jacquelyn Chapman and Johnathan Wisecarver helped give input into Venti-Now's simplified, low-cost ventilator design that could supply hospitals in impoverished areas during the pandemic. Photos/provided.
Wisecarver, who graduated from UC in May 2020, had a hand in the design of the ventilator and ensuring it meets ISO standards. He jumped at the chance to be involved with the nonprofit and use the skills he learned in his classes and co-ops – and learn from the seasoned engineers on the Venti-Now team – to help others during an uncertain time.
“I am just happy that I was able to jump in and immediately offer value to the team,” Wisecarver said. “Two months ago, you’re a student and planning out graduation, then a pandemic hits. You get an opportunity and before you know it, you’re helping design an emergency ventilator that will help save lives. What a way to enter the professional world.”
Venti-Now was launched with the goal to provide rapidly produced, safe, effective, and affordable emergency ventilators to fill the current and future needs of a pandemic. The company is working on the registration process to get donated units into Africa and Latin America, where access to ventilators is limited.
Most ventilators cost between $30,000 and 50,000, but Venti-Now’s version costs less than $5,000. As COVID-19 cases began to surge early this year, a huge effort launched in the United States to fill demand for ventilators, but there is a continuing global need for the devices.
Unlike most ventilators, Venti-Now’s product doesn’t require expensive oxygen tanks. Instead, it can be run off of compressor air, which makes it suitable for temporary emergency facilities and hospitals with or without air hookups. Many standard ventilators require trained personnel to operate, calibrate or fix the machines.
The device was designed to be easy to operate with minimal electronic components. It uses a pneumatic piston with a plunger that compresses a BVM (bag-valve-mask) bag; medical staff all over the world are familiar with how to operate a BVM. This unit takes that manual operation and automates it. The devices are automatically set to alarm at high or low pressure. By not requiring constant monitoring, it frees up medical staff to help other patients. Without access to ventilators in a developing country, it might be left to the patient’s family to manually squeeze the BVM bag to deliver lifesaving oxygen to the patient.
“I think this effort will have a positive impact on the rural and indigenous communities around the U.S., as well as impoverished countries. Ultimately, this relatively inexpensive device could be smoothly integrated into the healthcare systems in such countries and allow for nationwide healthcare improvements,” Chapman said.
Related Stories
UC’s commercialization navigator pilots tech transfer at 1819...
July 25, 2024
Housed within the University of Cincinnati’s 1819 Innovation Hub, the Technology Transfer team is vital to safeguarding and managing the intellectual property generated by UC’s researchers. Its mission is to translate UC's cutting-edge innovations into viable technologies by evaluating patentability and commercial viability, ensuring compliance and legal protection, recruiting and maintaining external partners, marketing technologies, negotiating license deals and identifying funding opportunities. This multifaceted approach ensures that groundbreaking discoveries from UC are positioned to reach the market, delivering substantial benefits that impact society.
UC hosts camp for children, teens who stutter
July 24, 2024
Children and teens who stutter have learned skills to help them communicate effectively, advocate for themselves and develop confidence about their communication abilities during a weeklong camp at the University of Cincinnati, Fox 19 reported.
Don't like your voice? There's an app for that.
July 24, 2024
WVXU's Cincinnati Edition talks to UC College of Engineering and Applied Science Associate Professor Vesna Novak about her new voice-coaching app.
