
Face masks may not protect against coronavirus
UC expert on aerosol studies explains performance of respiratory devices
University of Cincinnati scientist Sergey Grinshpun has tested the performance of respiratory protective devices against biological agents for nearly three decades.
Grinshpun, PhD, director of UC’s Center for Health Related Aerosol Studies, has a particular expertise in the effectiveness of face masks versus particulate respirators. He has been called upon in the midst of the coronavirus outbreak that began in China and is now spreading globally.
“When some major outbreak happens such as one with coronavirus or SARS or Ebola there is a lot of misinformation,” says Grinshpun, also a professor in the UC College of Medicine’s Department of Environmental and Public Health Sciences. “This relates to respiratory protective devices and what device to wear and also what protection level or efficiency you are paying for. People want to have something very light and comfortable, and they usually don’t like military style full-scale respiratory protective systems to carry around.”
Won’t a face mask protect me from coronavirus?
“The important difference is the face mask was not designed to protect a wearer, instead it is a barrier to droplets and spit generated by the wearer, which should protect others,” he explains.
Grinshpun says that individuals wearing certified N95 filtering facepiece respirators can screen about 95% of airborne particles if fitted correctly. Major workplaces including hospitals do a fit testing so that respirators are properly fitted, but many ordinary citizens have no idea how to properly wear the respirator. The lack of training and poor fit reduce the respirator effectiveness against diseases such as the one caused by the novel coronavirus.
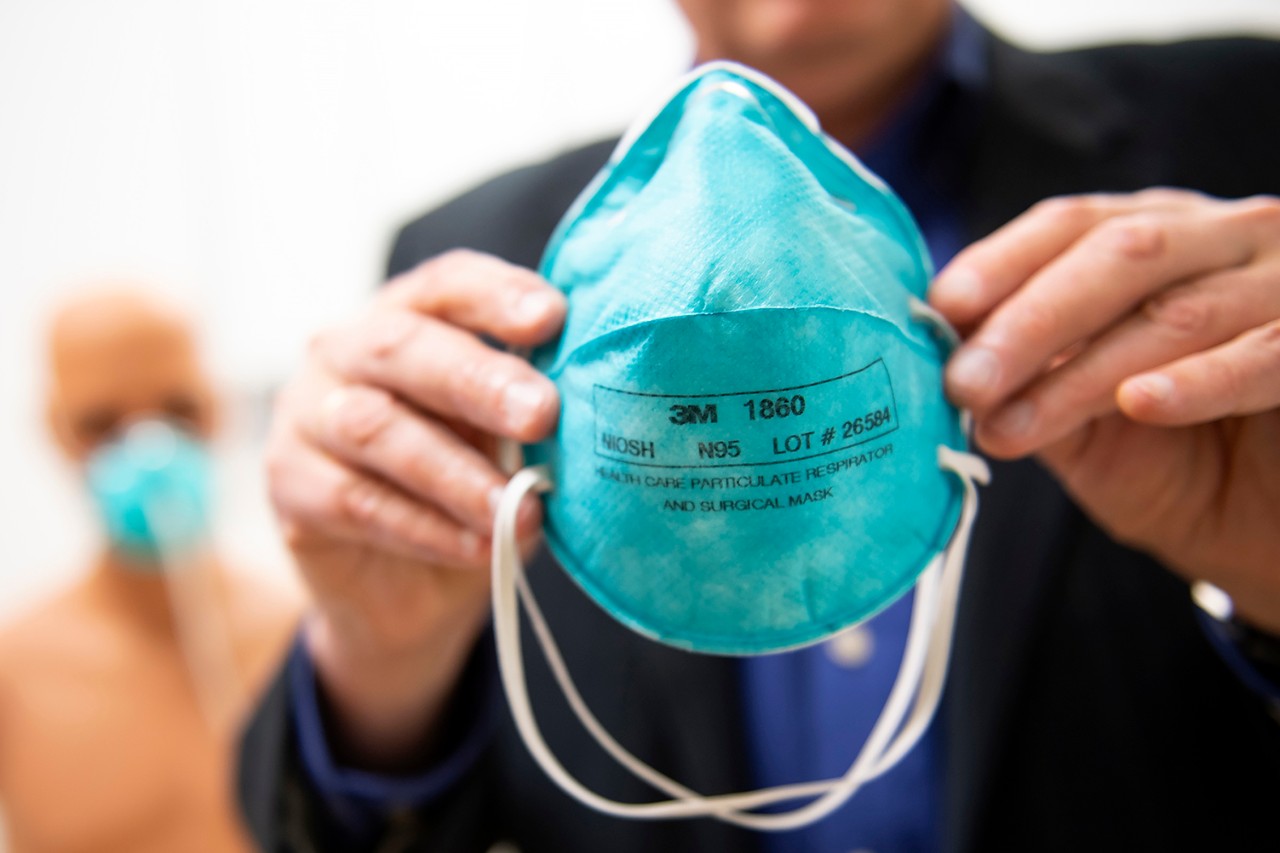
Shown is an N95 face filtering piece respirator. Photo by Colleen Kelley/UC Creative Services.
Grinshpun recalls researching the aftermath of Hurricane Katrina in New Orleans when many residents were given respirators because of mold and fungi outgrowth and its health concerns related to flooding. “When you put the respirator on your face you must make sure it fits. For instance, the nose clip was designed for a reason and must be used correctly. If not, particles penetrate through face-seal leakage and the N95 respirator may not offer the level of protection expected by its manufacturer.”
“We study the efficiency of face masks and various respirators on human subjects and breathing mannequins and in terms of penetration of particles through a conventional surgical mask, it may be as much as 50% or even greater,” he explains. “It is useless for people who want to wear this device to protect themselves. A surgeon in the operating room doesn’t want to sneeze or cough and infect the patient. A surgical mask may serve as an adequate barrier for this purpose, but what about viruses and bacteria aerosolized from the patient during surgery? If this aerosolization occurs, the surgeon and other medical staff are not well protected against it if wearing surgical masks. These masks may filter out very large droplets, but not tiny aerosolized particles.”
Virus particles often travel on water droplets and at some point the water evaporates and the particles shrink, Grinshpun says. At a smaller size, these particles can now penetrate the surgical mask.
Where can I find an N95 respirator?
Grinshpun says they are very short supply because of the demand in China and other places and the price, which used to be a little more than a dollar a piece has skyrocketed.
“This N95 was developed for workers in industry or medicine and not the general public,” he says. “The workers in this country are usually fit-tested. It’s done with a sophisticated apparatus which measures the concentration of particles inside and outside of a respirator donned on an individual performing certain exercises to determine the fit. If the fit is not acceptable, a worker may be offered a different size or type or respirator.”
Fit-testing can be expensive with the apparatus costing roughly $10,000, and requiring a qualified operator, says Grinshpun. Proper training should also be provided for wearers. “Now imagine if you want to take care of a large population in a short time. A respirator fit testing for the general public is an enormous task.”
Respiratory protection research and development is a booming area in terms of economics because the current global outbreak is probably not the last one.
Hear more about Grinsphun’s expertise on masks, respirators and coronavirus with the BBC. (Listen between the 9- and 12-minute marks.)
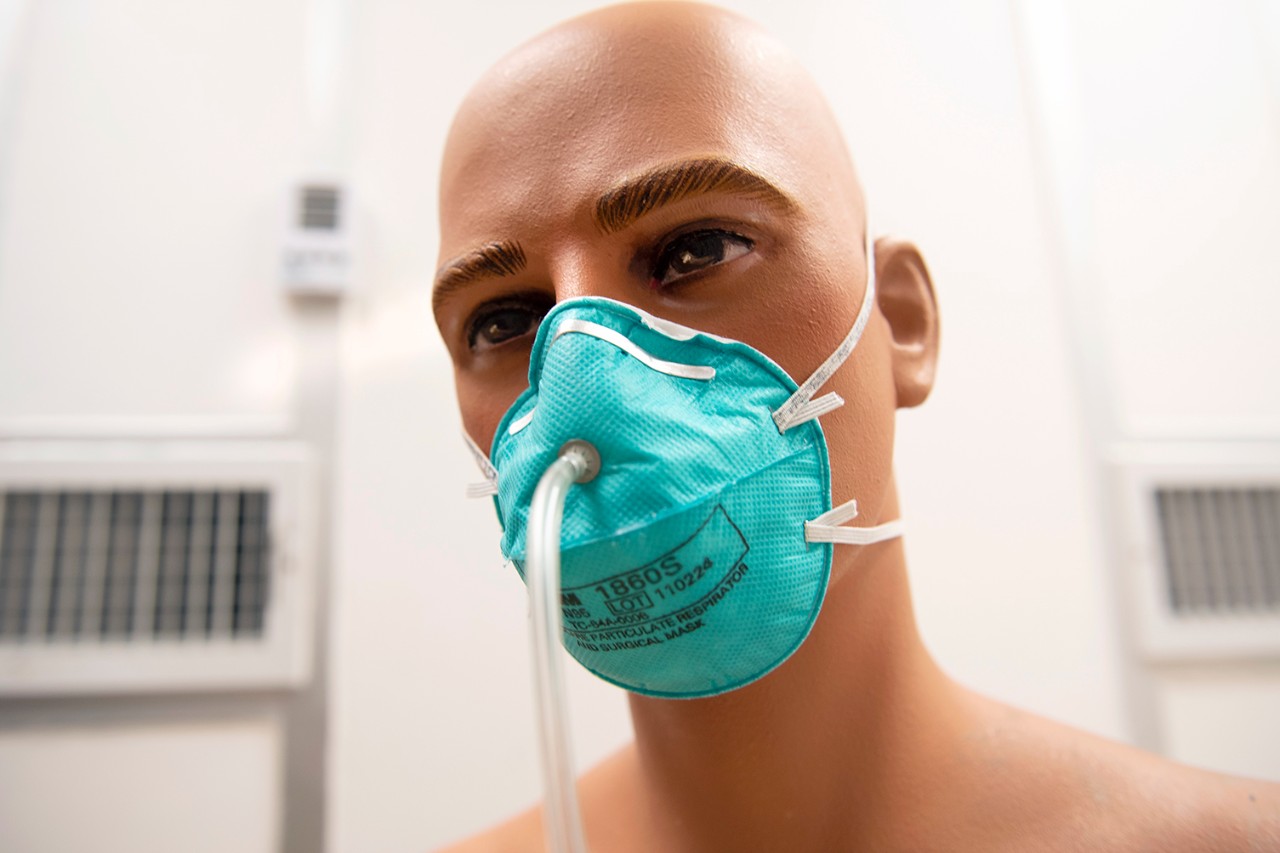
A mannequin in the UC Center for Health Related Aerosol Studies is fitted with an N95 filtering face piece respirator. Photo by Colleen Kelley/UC Creative Services.
Next Lives Here
The University of Cincinnati is classified as a Research 1 institution by the Carnegie Commission and is ranked in the National Science Foundation's Top-35 public research universities. UC's graduate students and faculty investigate problems and innovate solutions with real-world impact. Next Lives Here.
Featured photo at top: Sergey Grinshpun, PhD, in the UC Center for Health Related Aerosol Studies. Photo taken by Colleen Kelley/UC Creative Services.
Related Stories
At least two weather patterns increase headaches, UC study suggests
June 4, 2026
University of Cincinnati physicians and collaborators identified two specific weather patterns that increase headache and migraine risk and found the preventive medication fremanezumab (Ajovy) can reduce weather‑associated headaches. The findings will be presented at the American Headache Society Annual Scientific Meeting in Orlando.
UC researcher secures $3.3M grant to study microplastics’ impact on heart
June 2, 2026
The National Institute of Environmental Health Sciences awarded a $3.3M grant to University of Cincinnati researcher Hong‑Sheng Wang, PhD, to study how microplastics and nanoplastics affect cardiovascular health.
Taking a second look at surgery eligibility for patients with lung cancer who smoke
June 1, 2026
Researchers at the University of Cincinnati College of Medicine have found that patients who continue to smoke ahead of lung cancer surgery have a higher risk of pulmonary complications, but their short-term mortality rate is similar to patients who were able to stop smoking before surgery.. Their findings were published recently in the Journal of. American College of Surgeons
